How Pharmacists Engage in Patient Care Services Video
“Pharmacists have always been vital to the communities they serve. Today, pharmacists are integral members of healthcare teams, focusing on improving patient outcomes and delivering essential care. Many pharmacists are transitioning into roles with direct patient care responsibilities, becoming central figures in healthcare delivery.
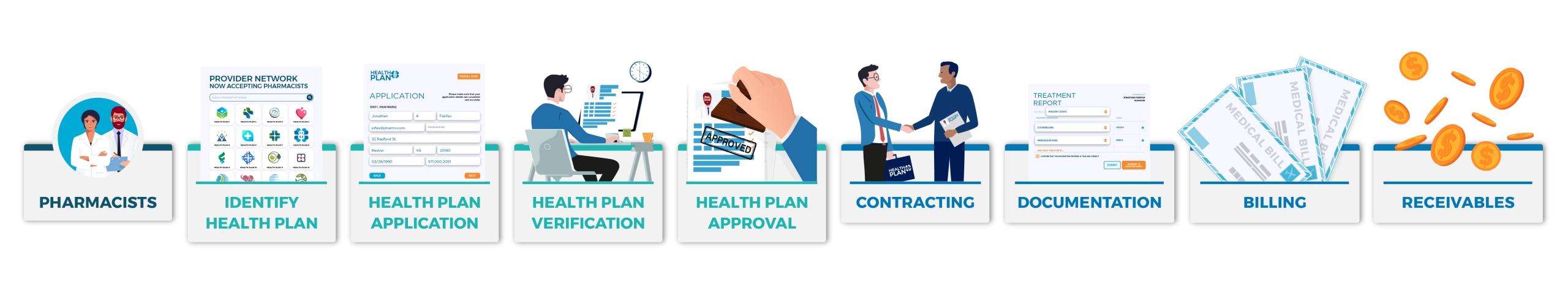
This video is your guide to understanding how you, as a pharmacist, can become enrolled as a healthcare provider within health plan provider networks to enable you to be paid for your patient care services. We’ll explain credentialing and walk you through the process of health plan enrollment.”
Pharmacists as Part of The Healthcare Team
“Access to primary care services has become a significant challenge for patients in many communities. The shortage of primary care providers has placed a greater focus on the value of community pharmacies as healthcare destinations. Pharmacists practicing in community pharmacies are trained and ready to fill the gap in ensuring patients have access to care.
Pharmacists serve as medication experts on healthcare teams and are increasingly providing direct patient care services. But how do pharmacists engage the healthcare system and get paid for services? How do they enroll with health plans as providers? How does contracting work? What do you need to know about patient care documentation, billing, and accounts receivable for medical claims?
The first step is understanding YOUR role in patient care. What services do you provide? Many pharmacists provide medication therapy management, chronic disease management, point-of-care testing, and preventive services like immunizations.
It’s equally necessary to understand the scope of practice as defined by your state’s pharmacy laws. This helps determine what services you’re authorized to provide and bill for. If you’re unsure, reach out to your state pharmacy association for guidance.”
The Health Plan Enrollment Process
“The first step is to ensure you have obtained your individual National Provider Identification Number or NPI number. This is a unique 10-digit identification code utilized in all HIPPA electronic transactions, including with payors. It is free to apply and is unique to you for the lifetime of your career.
The next step is to identify potential health plans in your local market that allow pharmacists to enroll as healthcare providers. It’s important to consider health plans with sufficient presence in your geographic region. Your state association may be able to provide guidance on how to find health plans in your market that engage pharmacists as providers.
Once you’ve identified health plans, go to their network enrollment website to begin the provider network enrollment application process. Submit an individual application to your chosen health plan. Note that each health plan or health insurance company may have a slightly different application process. However, be sure that your application details are accurate. Even a small error may greatly delay the process.
During the application process, health plans request that you provide your verified credentials. Credentialing is a detailed process that verifies your professional qualifications, including licensure, education, and work history, as well as any discipline or sanctions. This information is verified using primary sources like your state Board of Pharmacy and the National Practitioner Data Bank.
Health plans may complete the credentialing process on their own, but most rely on third-party experts known as Credentials Verification Organizations (or CVOs). These organizations, like Pharmacy Profiles, maintain centralized credentialing repositories that simplify the process—especially for pharmacists applying to multiple provider networks. Pharmacy Profiles is certified by the National Committee for Quality Assurance (NCQA, for short), which sets rigorous industry standards for accuracy, security, and efficiency.
Once your applications have been submitted, health plans will conduct a verification and approval process. A health plan credentialing committee will review your application to ensure you meet their standards before granting approval.”
Navigating Network Services
“Once you’re part of a health plan’s network, you’ll need to understand how to work effectively within their network.
Generally, health plans contract with pharmacies or pharmacy networks rather than directly with individual pharmacists. Therefore, as a pharmacist, you will not likely be directly responsible for managing billing and receivables. However, you will play an important role in ensuring that you accurately code and document the services you provide. Accurate coding and thorough documentation are essential. They not only help you get paid but also establish the strong record required for compliance and audits.
Many pharmacies and pharmacy networks partner with a medical billing company to help streamline getting complete claims to the health plans, and receiving remittance feedback to finalize the billing and payment cycles.”
“By following these steps, you can position yourself as an integral member of the healthcare team and be paid for your services. This opens doors to new opportunities that leverage your expertise to provide patient care services. Visit www.PharmacyProfiles.com to learn more and claim your profile.”